How to Read Eeg Coherence Measure Table
This guide demonstrates how to read an ECG using a systematic approach. If yous want to put your ECG estimation knowledge to the test, cheque out our ECG quiz on the Geeky Medics quiz platform.
You may also be interested in our ECG flashcard deck which can be purchased as office of our collection of thou+ OSCE flashcards.
Confirm details
Before beginning ECG interpretation, yous should cheque the following details:
- Confirm the name and engagement of nascency of the patient matches the details on the ECG.
- Check the date and time that the ECG was performed.
- Check the calibration of the ECG (usually 25mm/s and 10mm/1mV).
Y'all might as well be interested in our OSCE Flashcard Drove which contains over 2000 flashcards that cover clinical examination, procedures, communication skills and data interpretation.
Centre rate
What's a normal developed heart rate?
- Normal: 60-100 bpm
- Tachycardia: > 100 bpm
- Bradycardia: < sixty bpm
Regular heart rhythm
If a patient has a regular heart rhythm their heart charge per unit can exist calculated using the following method:
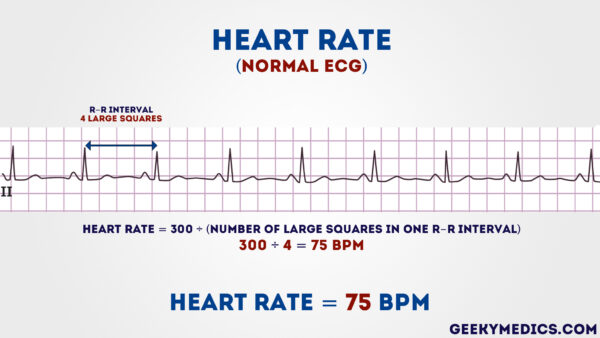
- Count the number of large squares present within i R-R interval.
- Split 300 by this number to summate heart rate.
Eye rate adding example
- 4 large squares in an R-R interval
- 300/4 = 75 beats per minute
Irregular eye rhythm
If a patient's heart rhythm is irregular the offset method of centre rate calculation doesn't piece of work (every bit the R-R interval differs significantly throughout the ECG). As a event, you demand to apply a different method:
- Count the number of complexes on the rhythm strip (each rhythm strip is typically 10 seconds long).
- Multiply the number of complexes by 6 (giving you lot the average number of complexes in i infinitesimal).
Heart rate calculation example
- 10 complexes on a rhythm strip
- ten 10 half dozen = 60 beats per minute
Eye rhythm
A patient's heart rhythm can be regular or irregular.
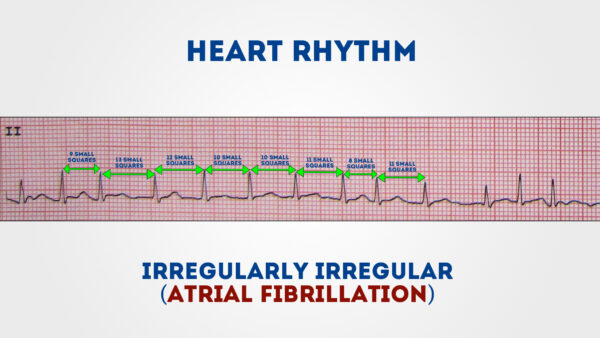
Irregular rhythms can be either:
- Regularly irregular (i.e. a recurrent design of irregularity)
- Irregularly irregular (i.e. completely disorganised)
Mark out several consecutive R-R intervals on a piece of newspaper, and so move them along the rhythm strip to check if the subsequent intervals are similar.
Hint
If you are suspicious that in that location is some atrioventricular block (AV block), map out the atrial rate and the ventricular rhythm separately (i.e. mark the P waves and R waves). Equally you move forth the rhythm strip, y'all tin then run into if the PR interval changes, if QRS complexes are missing or if there is complete dissociation between the ii.
Cardiac centrality
Cardiac axis describes the overall direction of electrical spread within the heart.
In a healthy individual, the axis should spread from eleven o'clock to 5 o'clock.
To determine the cardiac axis you need to await at leads I, 2 and Three.
Read our cardiac axis guide to learn more.
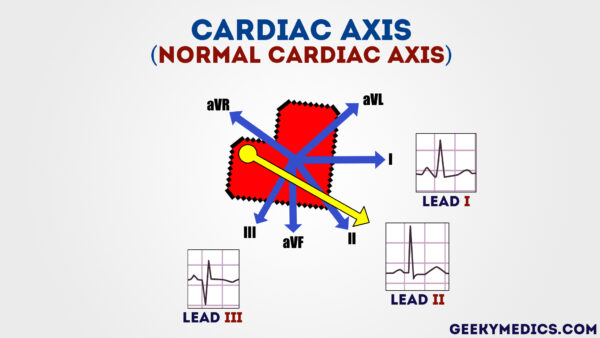
Normal cardiac axis
Typical ECG findings for normal cardiac axis:
- Atomic number 82 II has the most positive deflection compared to leads I and III.
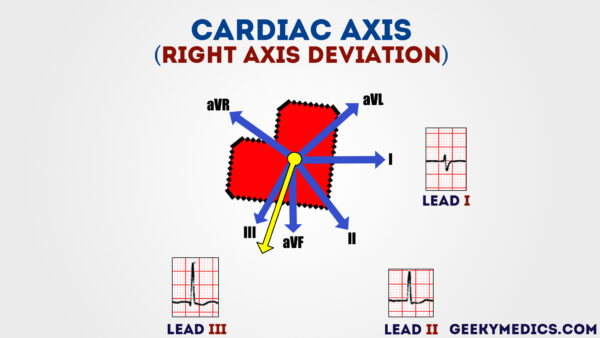
Correct centrality deviation
Typical ECG findings for correct axis deviation:
- Lead III has the most positive deflection and lead I should exist negative.
- Right axis deviation is associated with right ventricular hypertrophy.
Left axis deviation
Typical ECG findings for left centrality divergence:
- Lead I has the most positive deflection.
- Leads Ii and Iii are negative.
- Left centrality difference is associated with middle conduction abnormalities.

P waves
The side by side step is to await at the P waves and answer the post-obit questions:
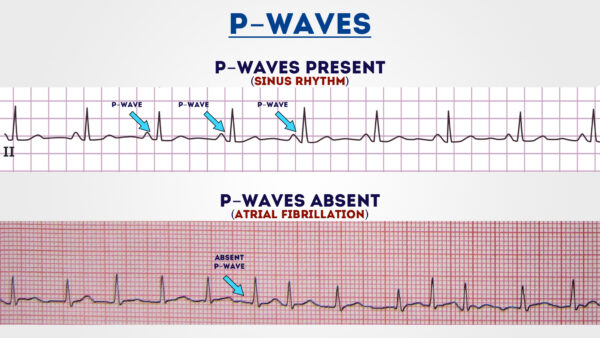
ane. Are P waves present?
2. If and then, is each P wave followed by a QRS circuitous?
3. Exercise the P waves expect normal? – check elapsing, management and shape
4. If P waves are absent, is there whatsoever atrial activity?
- Sawtooth baseline → flutter waves
- Cluttered baseline → fibrillation waves
- Flat line → no atrial activeness at all
Hint
If P waves are absent-minded and there is an irregular rhythm information technology may advise a diagnosis of atrial fibrillation.
PR interval
The PR interval should be between 120-200 ms(3-5 pocket-size squares).
Prolonged PR interval (>0.ii seconds)
A prolonged PR interval suggests the presence of atrioventricular filibuster (AV block).
First-degree heart block (AV block)
First-caste heart block involves a fixed prolonged PR interval (>200 ms).

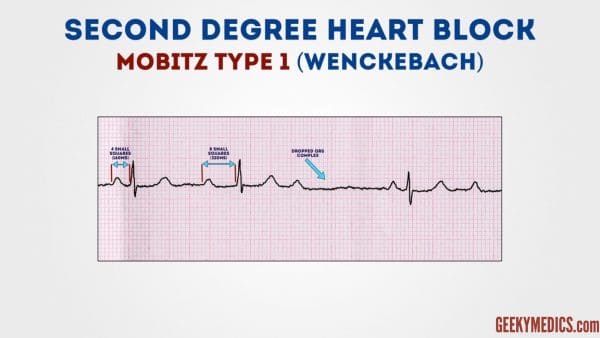
Second-degree heart cake (type 1)
Second-degree AV block (blazon 1) is also known asMobitz blazon i AV block orWenckebach phenomenon.
Typical ECG findings in Mobitz blazon i AV block includeprogressive prolongation of the PR interval until eventually the atrial impulse is non conducted and theQRS complex is dropped.
AV nodal conductionresumes with the side by side beat out and the sequence of progressive PR interval prolongation and the eventual dropping of a QRS circuitousrepeats itself.
Second-degree heart block (type 2)
Second-degree AV block (blazon 2) is besides known every bitMobitz type 2 AV block.
Typical ECG findings in Mobitz blazon 2 AV cake include a consistent PR interval duration withintermittently dropped QRS complexes due to a failure of conduction.
The intermittent dropping of the QRS complexes typically follows arepeating cycle of every3rd (3:1 block) orquaternary (4:1 block)P wave.

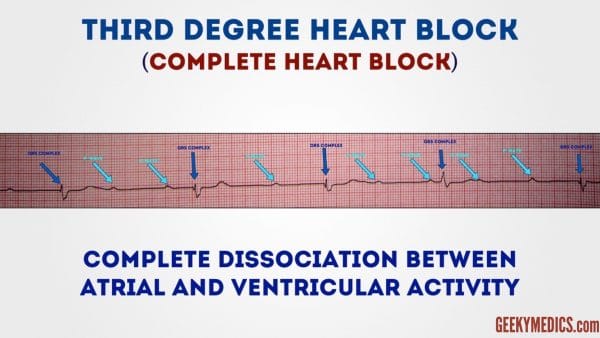
Tertiary-degree center block (complete heart block)
Third-degree (complete) AV block occurs when there is no electrical communicationbetween theatria andventricles due to a complete failure of conduction.
Typical ECG findings include thepresence of P waves andQRS complexes that haveno association with each other, due to the atria and ventricles operation independently.
Cardiac function is maintained by ajunctional orventricularpacemaker.
Narrow-complex escape rhythms (QRS complexes of <0.12 seconds duration) originateto a higher place the bifurcation of thebundle of His.
Broad-complex escape rhythms (QRS complexes >0.12 seconds elapsing) originate frombelow the bifurcation of the bundle of His.
Tips for remembering types of heart block
To help remember the diverse types of AV cake, it is useful to know the anatomical location of the block within the conducting system.
Commencement-caste AV block:
- Occurs between the SA node and the AV node (i.e. within the atrium).
2d-caste AV block:
- Mobitz I AV block (Wenckebach) occurs IN the AV node (this is the only piece of conductive tissue in the heart which exhibits the power to conduct at different speeds).
- Mobitz II AV block occurs After the AV node in the bundle of His or Purkinje fibres.
3rd-degree AV cake:
- Occurs at or after the AV node resulting in a complete blockade of distal conduction.
Shortened PR interval
If the PR interval is shortened, this can mean one of two things:
- But, the P moving ridge is originating from somewhere closer to the AV node so the conduction takes less time (the SA node is not in a fixed place and some people's atria are smaller than others).
- The atrial impulse is getting to the ventricle by a faster shortcut instead of conducting slowly across the atrial wall. This is an accessory pathway and tin can exist associated with a delta wave (see beneath which demonstrates an ECG of a patient with Wolff Parkinson White syndrome).
QRS complex
When assessing a QRS complex, you lot need to pay attending to the following characteristics:
- Width
- Height
- Morphology
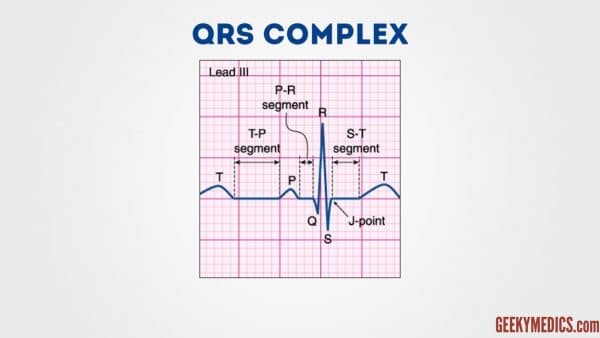
Width
Width can exist described as NARROW (< 0.12 seconds) or Wide (> 0.12 seconds):
- A narrow QRS complex occurs when the impulse is conducted down the package of His and the Purkinje fibre to the ventricles. This results in well organised synchronised ventricular depolarisation.
- A broad QRS complex occurs if there is an aberrant depolarisation sequence – for case, a ventricular ectopic where the impulse spreads slowly beyond the myocardium from the focus in the ventricle. In contrast, an atrial ectopic would result in a narrow QRS complex because it would conduct down the normal conduction system of the heart. Similarly, a parcel co-operative block results in a wide QRS circuitous because the impulse gets to one ventricle quickly down the intrinsic conduction organization then has to spread slowly across the myocardium to the other ventricle.
Top
Height can be described equally either Small or Tall:
- Pocket-sized complexes are defined as < 5mm in the limb leads or < x mm in the chest leads.
- Tall complexes imply ventricular hypertrophy (although tin can be due to body habitus e.g. tall slim people). There are numerous algorithms for measuring LVH, such as the Sokolow-Lyon alphabetize or the Cornell index.
Morphology
To assess morphology, you demand to assess the individual waves of the QRS complex.
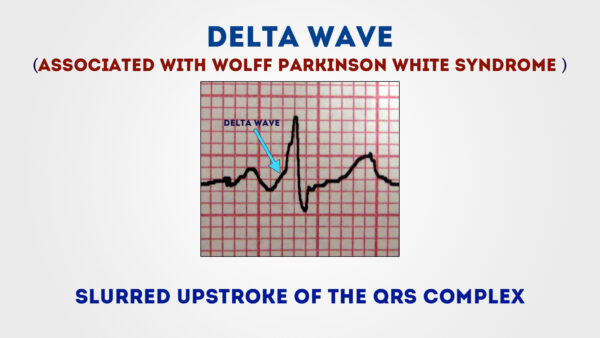
Delta wave
The mythical 'delta wave' is a sign that the ventricles are being activated before than normal from a betoken distant to the AV node. The early activation then spreads slowly across the myocardium causing the slurred upstroke of the QRS complex.
Note – the presence of a delta wave does Not diagnose Wolff-Parkinson-White syndrome. This requires testify of tachyarrhythmias AND a delta moving ridge.

Q-waves
Isolated Q waves can be normal.
A pathological Q wave is > 25% the size of the R moving ridge that follows it or > 2mm in pinnacle and > 40ms in width.
A single Q wave is non a cause for business – look for Q waves in an unabridged territory (eastward.g. anterior/junior) for evidence of previous myocardial infarction.

R and S waves
Assess the R wave progression across the chest leads (from small in V1 to big in V6).
The transition from S > R wave to R > Southward wave should occur in V3 or V4.
Poor progression (i.e. South > R through to leads V5 and V6) tin be a sign of previous MI but can also occur in very large people due to poor lead position.
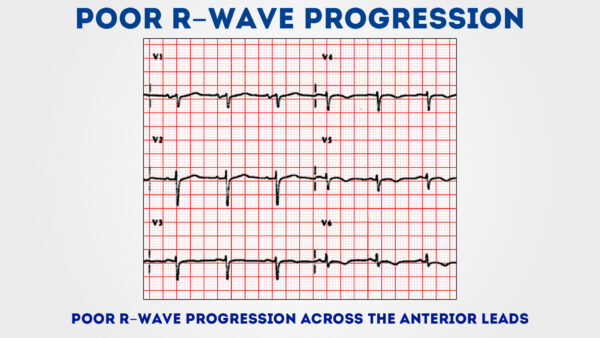
J point segment
The J point is where the S wave joins the ST segment.
This bespeak can be elevated resulting in the ST segment that follows it too existence raised (this is known equally "high take-off").
High take-off (or benign early repolarisation to give its full title) is a normal variant that causes a lot of malaise and confusion as information technology LOOKS like ST elevation.
Fundamental points for assessing the J point segment:
- Benign early repolarisation occurs mostly under the age of 50 (over the age of 50, ischaemia is more than mutual and should be suspected start).
- Typically, the J indicate is raised with widespread ST top in multiple territories making ischaemia less likely.
- The T waves are also raised (in contrast to a STEMI where the T wave remains the same size and the ST segment is raised).
- The ECG abnormalities exercise non change! During a STEMI, the changes will evolve – in beneficial early on repolarisation, they will remain the aforementioned.
ST segment
The ST segment is the part of the ECG between the end of the S wave and the start of the T moving ridge.
In a healthy individual, it should be an isoelectric line (neither elevated nor depressed).
Abnormalities of the ST segment should be investigated to rule out pathology.

ST-tiptop
ST-elevation is significant when it is greater than ane mm (i minor square)in 2 or more contiguous limb leads or >2mm in 2 or more breast leads.
It is most commonly caused past astute full-thickness myocardial infarction.
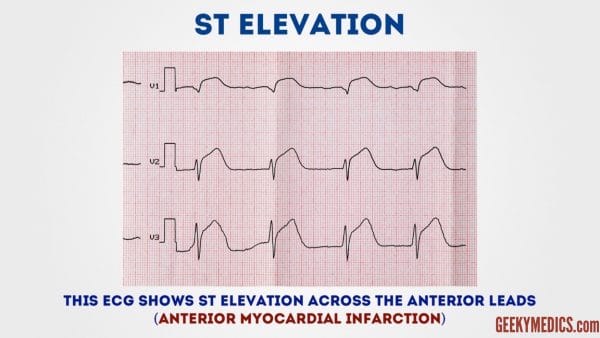
ST low
ST depression ≥ 0.5 mm in ≥ 2 face-to-face leads indicates myocardial ischaemia.
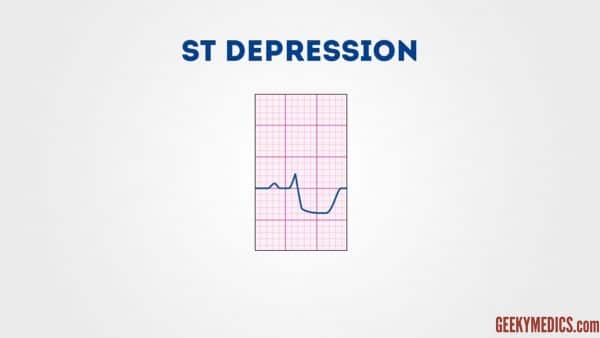
T waves
T waves represent repolarisation of the ventricles.
Tall T waves
T waves are considered tall if they are:
- > 5mm in the limb leads AND
- > 10mm in the chest leads (the aforementioned criteria as 'small' QRS complexes)
Alpine T waves can be associated with:
- Hyperkalaemia ("tall tented T waves")
- Hyperacute STEMI

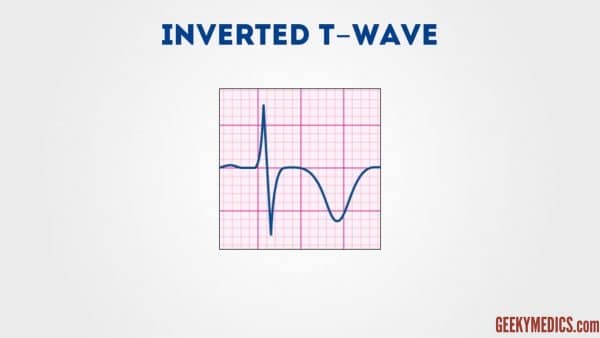
Inverted T waves
T waves are normally inverted in V1 and inversion in lead III is a normal variant.
Inverted T waves in other leads are a nonspecific sign of a broad variety of weather condition:
- Ischaemia
- Packet branch blocks (V4-vi in LBBB and V1-V3 in RBBB)
- Pulmonary embolism
- Left ventricular hypertrophy (in the lateral leads)
- Hypertrophic cardiomyopathy (widespread)
- General illness
Around 50% of patients admitted to ITU have some evidence of T wave inversion during their stay.
Observe the distribution of the T wave inversion (east.chiliad. anterior/lateral/posterior leads).
You must have this ECG finding and use it in the context of your patient.
Biphasic T waves
Biphasic T waves have ii peaks and can be indicative of ischaemia and hypokalaemia.

Flattened T waves
Flattened T waves are a non-specific sign, that may represent ischaemia or electrolyte imbalance.

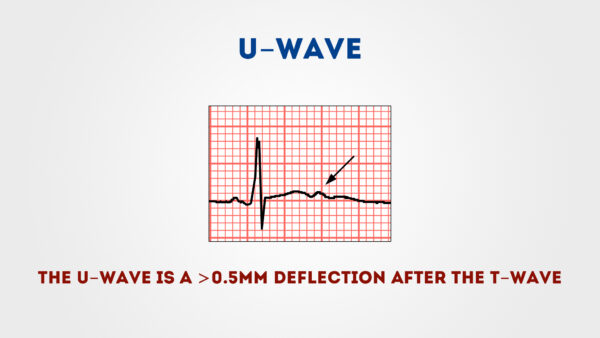
U waves
U waves are not a common finding.
The U wave is a > 0.5mm deflection after the T wave best seen in V2 or V3.
These become larger the slower the bradycardia – classically U waves are seen in various electrolyte imbalances, hypothermia and secondary to antiarrhythmic therapy (such as digoxin, procainamide or amiodarone).
Certificate your estimation
You should document your interpretation of the ECG in the patient's notes (cheque out our guide to documenting an ECG).
References
- James Heilman, Dr.. Fast atrial fibrillation. Licence: CC By-SA three.0.
- Michael Rosengarten BEng, Physician.McGill. Right axis departure. Licence: CC Past-SA 3.0.
- James Heilman, MD. Mobitz type two AV block. Licence: CC By-SA 3.0.
- James Heilman, MD. Consummate centre block. Licence: CC Past-SA 3.0.
- James Heilman, MD. Delta wave. Licence: CC BY-SA 3.0.
- Michael Rosengarten BEng, Medico.McGill. Q-waves. Licence: CC BY-SA three.0.
- Michael Rosengarten BEng, Doctor.McGill. Poor R-moving ridge progression. Licence: CC Past-SA three.0.
- Michael Rosengarten BEng, MD.McGill. Tall tented T-waves. Licence: CC Past-SA 3.0.
- CardioNetworks. T-wave morphology. Licence: CC By-SA 3.0.
- James Heilman, Md. U-wave. Licence: CC By-SA 3.0.
- Michael Rosengarten BEng, MD.McGill. Left centrality deviation. Licence: CC By-SA 3.0.
Source: https://geekymedics.com/how-to-read-an-ecg/

Belum ada Komentar untuk "How to Read Eeg Coherence Measure Table"
Posting Komentar